Tom Koch on Ebola and the “new” epidemic
“Ebola and the ‘new’ epidemic” by Tom Koch
Mindless but intelligent, viruses and bacteria want what we all want: to survive, evolve, and then, to procreate. That’s been their program since before there were humans. From the first influenza outbreak around 2500 BC to the current Ebola epidemic, we have created the conditions for microbial evolution, hosted their survival, and tried to live with the results.
These are early days for the Ebola epidemic, which was for some years constrained to a few isolated African sites, but has now advanced from its natal place to several countries, with outbreaks elsewhere. Since the first days of influenza, this has always been the viral way. Born in a specific locale, the virus hitches itself to a traveler who brings it to a new and fertile field of humans. The “epidemic curve,” as it is called, starts slowly but then, as the virus spreads and travels, spreads and travels, the numbers mount.
Hippocrates provided a fine description of an influenza pandemic in 500 BC, one that reached Greece from Asia. The Black Death that hastened the end of the Middle Ages traveled with Crusaders and local traders, infecting the then-known world. Cholera (with a mortality rate of over thirty percent) started in India in 1818 and by 1832 had infected Europe and North America.
Since the end of the seventeenth century, we’ve mapped these spreads in towns and villages located in provinces and nations. The first maps were of plague, but in the eighteenth century that scourge was replaced in North American minds by yellow fever, which in turn, was replaced by the global pandemic of cholera (and then at the end of the century came polio).
In attempting to combat these viral outbreaks, the question is one of scale. Early cases are charted on the streets of a city, the homes of a town. Can they be quarantined and those infected separated? And then, as the epidemic grows, the mapping pulls back to the nations in which those towns are located as travelers, infected but as yet not symptomatic, move from place to place. Those local streets become bus and rail lines that become, as a pandemic begins, airline routes that gird the world.
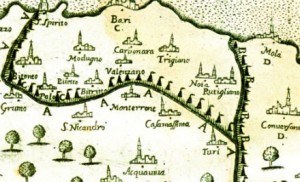
There are lots of models for us to follow here. In the 1690s, Filipo Arrieta mapped a four-stage containment program that attempted to limit the passage of plague through the province of Bari, Italy, where he marshaled the army to create containment circles.
Indeed, quarantines have been employed, often with little success, since the days of plague. The sooner they are put in place, the better they seem to be. They are not, however, foolproof.
Complacently, we have assumed that our expertise at genetic profiling would permit rapid identification and the speedy production of vaccines or at least curative drugs. We thought we were beyond viral attack. Alas, our microbial friends are faster than that. By the time we’ve genetically typed the virus and found a biochemical to counter it, it will have, most likely, been and gone. Epidemiologists talk about the “epidemic curve” as a natural phenomenon that begins slowly, rises fiercely, and then ends.
We have nobody to blame but ourselves.
Four factors promote the viral and bacterial evolution that results in pandemic diseases and their spread. First, there is the deforestation and man-made ecological changes that upset natural habitats, forcing microbes to seek new homes. Second, urbanization brings people together in dense fields of habitation that become the microbe’s new hosts—when those people live in poverty, the field is even better. Third, trade provides travelers to carry microbes, one way or another, to new places. And, fourth and finally, war always promotes the spread of disease among folk who are poor and stressed.
We have created this perfect context in recent decades and the result has been a fast pace of viral and bacterial evolution to meet the stresses we impose and the opportunities we present as hosts. For their part, diseases must balance between virulence—killing the person quickly—and longevity. The diseases that kill quickly usually modify over time. They need their hosts, or something else, to help them move to new fields of endeavor. New diseases like Ebola are aggressive adolescents seeking the fastest, and thus deadliest, exchanges.
Will it become an “unstoppable” pandemic? Probably not, but we do not know for certain; we don’t know how Ebola will mutate in the face of our plans for resistance.
What we do know is that as anxiety increases the niceties developed over the past fifty years of medical protocol and ethics will fade away. There will now be heated discussions surrounding “ethics” and “justice,” as well as practical questions of quarantine and care. Do we try experimental drugs without the normal safety protocol? (The answer will be … yes, sooner if not later.) If something works and there is not enough for all, how do we decide to whom it is to be given first?
For those like me who have tacked diseases through history and mapped their outbreaks in our world, Ebola, or something like it, is what we have feared would come. And when Ebola is contained it will not be the end. We’re in a period of rapid viral and bacterial evolution brought on by globalization and its trade practices. Our microbial friends will, almost surely, continue to take advantage.
For more from Tom Koch on mapping the containment of pandemics and Ebola in particular, visit his recent piece for Remedia, here.
***
Tom Koch is a medical geographer, ethicist, and the author of a number of papers in the history of medicine and disease, who has earned degrees from Clark University and the University of British Columbia. His most recent book in this field was Disease Maps: Epidemics on the Ground, published by University of Chicago Press.